Greetings, Science Explorers!
Today we’re taking a deep dive into the incredible world of our body’s microscopic insulin factories – the pancreatic beta cells. You’re going to learn how they produce insulin, why it matters, and what happens when we eat. Let’s jump right in!
The First Passage of Insulin
It all starts in the pancreas, where about 50%-60% of insulin produced by the beta cells makes a quick pit-stop in the liver before reaching the rest of the body. This detour allows the liver to filter out some insulin, ensuring that insulin concentration in the portal vein (which supplies the liver) is higher than in other parts of the body.
The Role of Basal Insulin
You see, we don’t just need insulin when we eat. Our bodies need a constant supply of insulin, even when fasting, to maintain a state of “basal euglycaemia”, essentially, a stable blood sugar level. So, our pancreatic beta cells always produce some insulin, even when we aren’t munching on a sandwich or enjoying a bowl of soup.
Insulin Release: More Than Just Glucose
While glucose (the sugar we get from food) is a major trigger for insulin release, it’s not the only player on the field. Other nutrients like different sugars, amino acids, and fatty acids also contribute. Plus, hormones and neural factors join the game, all playing crucial roles in maintaining our blood sugar balance.
GLUTs: The Gatekeepers
Here’s where things get a bit sci-fi! Our pancreatic beta cells use special proteins called GLUTs (glucose transporters) to decide how much glucose gets into the cells. In humans, these gatekeepers are usually GLUT1 and GLUT3, while in rodents, it’s GLUT2. The primary role of these transporters is to facilitate the diffusion of glucose into cells, regardless of how much sugar is around them.
Interestingly, these GLUTs are not all created equal. GLUT1 and GLUT3 have a high affinity for glucose but can only handle a limited amount at a time. On the other hand, GLUT2 is less picky but can handle a higher glucose load. This diversity allows for a more flexible response to varying blood glucose levels.
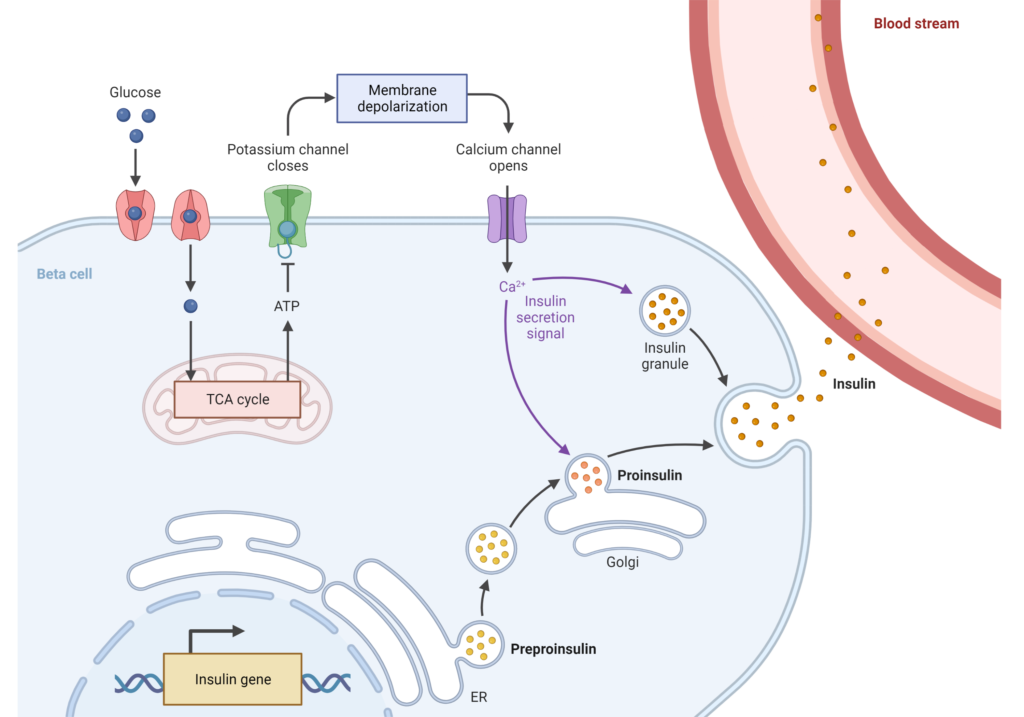
The Journey of Glucose Inside the Beta Cell
Once glucose has entered the cell, it’s greeted by an enzyme called glucokinase (GCK). GCK kickstarts the breakdown of glucose, turning it into glucose 6 phosphate. This molecule then goes on a metabolic journey through a process called glycolysis, ending up as pyruvate, which is used in the mitochondria (our cell’s powerhouses) to produce ATP, our body’s energy currency.
As ATP levels rise, they shut down the KATP channels on the cell surface, which triggers a sequence of events that opens the gates for calcium ions. The surge of calcium leads to insulin-containing secretory granules being released into the bloodstream.
The Symphony of Insulin Secretion
In addition to ATP, several other molecules generated during glucose metabolism act as signals to further amplify insulin secretion. It’s like a finely tuned symphony, with every player contributing to the grand performance of insulin release.
In conclusion, insulin secretion is an intricate dance involving various actors and stages. It’s a process of fine balance, amazing precision, and phenomenal coordination that helps keep us healthy and energetic throughout the day. So next time you’re enjoying your favourite meal, take a moment to appreciate the fantastic work being done by your tiny insulin factories!
Until next time, stay curious and keep exploring!